FIFTEEN children under 15 have now died from killer Strep A complication this winter as health chiefs say knock-on effects of Covid lockdowns may be to blame for unusually big outbreak
- Victims include under-10s in England, Northern Ireland and Wales
- Strep A can cause infections, including impetigo, scarlet fever and strep throat
- In extremely rare cases, the bacteria can trigger a life-threatening complication
Fifteen children have now died from Strep A in Britain this winter as the killer bug outbreak rumbles on.
Victims include Stella-Lilly McCorkindale, a five-year-old girl from Northern Ireland, Hannah Roap, a 'bubbly' seven-year-old from Wales, and Muhammad Ibrahim Ali, a four-year-old boy from Buckinghamshire.
Strep A bacteria can cause a myriad of infections, including impetigo, scarlet fever and strep throat. The vast majority of cases are mild.
In extremely rare cases, however, the bacteria can penetrate the blood and trigger a life-threatening complication. Almost 170 children have been hit by invasive Group A Strep (iGAS) already this season, health chiefs confirmed today.


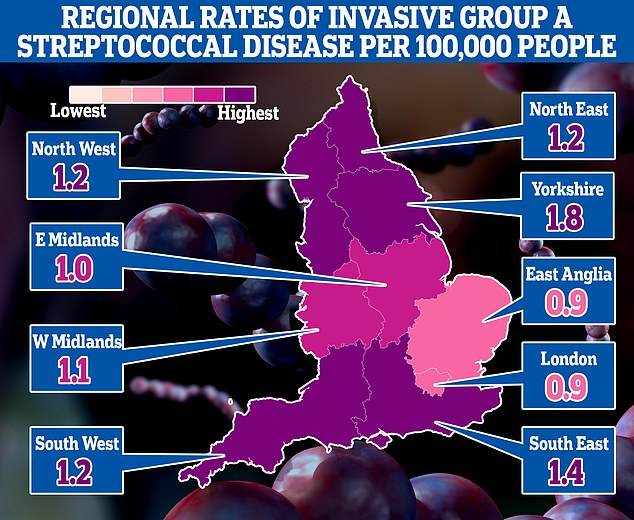
The map shows the rate of iGAS per 100,000 people in England between September 12 and December 4. Rates were highest in Yorkshire (1.8) and the South East (1.4)
Strep A outbreaks tend start to gather speed in the New Year, before peaking in the spring. But cases have taken off earlier than usual this year.
Overall, 659 cases of iGAS have been detected in England so far this season, 60 of which have been fatal.
UK Health Security Agency (UKHSA) data suggests five times as many infants have been struck down this winter, compared to before Covid.
Some 169 cases of iGAS in under-14s were recorded between September 12 and December 4.
For comparison, 431 developed the complication during the entirety of 2017/18 — considered the last 'bad' year.
Among children this year, cases are most common among one to four-year-olds (85), followed by five to nine-year-olds (60), under-ones (13) and 10 to 14-year-olds (11).
In England, there have been 13 iGAS deaths among under-15s.
There has also been one fatality in Northern Ireland and another in Wales, bringing the UK total to 15.
In the last bad season in England, there were 27 deaths among children.
But the case fatality ratio — the number of confirmed infections that die — is in-line with previous years, the UKHSA said.
And the majority of England's total 659 cases continue to be among adults, with 490 infections and 47 fatalities among over-18s since mid-September.
Some 23 of the deaths have been among over-75s.
Rates of iGAS are highest in Yorkshire (1.8 cases per 100,000 people), followed by the South East (1.4). Levels were lowest in the East of England and London (0.9).
The UKHSA said there is usually a surge in iGAS cases every three to four years but social distancing during the Covid pandemic 'may have interrupted this cycle and explain the current increase'.
It said: 'The increase is likely to reflect increased susceptibility to these infections in children due to low numbers of cases during the pandemic.'
High rates of other respiratory viruses — including flu, RSV and norovirus — may be putting children at higher risk of co-infections with Strep A, leaving them more susceptible to severe illness, the UKHSA suggested.
There is no evidence that a new strain of iGAS is behind the outbreak but scientists are investigating what other factors could be behind the spike, it said.
They are also examining an increase in lower respiratory tract iGAS infections in children over recent weeks, particularly emphysema — damage to the air sacs in the lungs.
Meanwhile, the UKHSA has logged 6,601 cases of scarlet fever — which is caused by Strep A. This is two-and-a-half times higher than the 2017/18 season.
More than 1,000 cases were reported in the most recent week alone.
It is 'important' that scarlet fever cases are 'treated promptly with antibiotics to limit further spread and reduce risk of potential complications' among those infected and their close contacts, the UKHSA said.
Phenoxymethylpenicillin, amoxicillin and clarithromycin are three antibiotics used to treat Strep A infections.
Health chiefs have advised doctors to have a 'low threshold' for prescribing these to youngsters who have suspected Strep A, raising concerns that this could lead to antibiotic resistance — when the treatment become less effective against bacteria due to overuse.
But the UKHSA today emphasised that antibiotic resistance is not on the rise.
Dr Colin Brown, deputy director at the UKHSA, said: 'Scarlet fever and "strep throat" are common childhood illnesses that can be treated easily with antibiotics.
'Please visit NHS.uk, contact 111 online or your GP surgery if your child has symptoms of this infection so they can be assessed for treatment.
'Very rarely, the bacteria can get into the bloodstream and cause more serious illness called invasive Group A strep.
'We know that this is concerning for parents, but I want to stress that while we are seeing an increase in cases in children, this remains very uncommon.'

The UKHSA has logged 6,601 cases of scarlet fever — which is caused by Strep A — between September 12 and December 4 (green line). For comparison, just 2,538 cases had been reported by this point in 2017/18 (thin blue line), which was considered a 'bad' season

Between September 12 and December 4, the UKHSA was notified of 659 iGAS cases (grey line). Rates are currently higher than the previous five winters
He added: 'There a lots of winter bugs circulating that can make your child feel unwell, that mostly aren’t cause for alarm.
'However, make sure you talk to a health professional if your child is getting worse after a bout of scarlet fever, a sore throat or respiratory infection – look out for signs such as a fever that won’t go down, dehydration, extreme tiredness and difficulty breathing.'
It comes after parents and pharmacists have told of their difficulties accessing vital antibiotics used to treat Strep A infections.
The Prime Minister and Health Secretary have insisted the drugs are not in short supply, however.
Steve Barclay admitted that individual GP clinics may have supply issues but noted that there are 'well-established procedures' for moving stock around the country when there is a 'surge in demand'.
A Department of Health spokesperson today said that there is 'no supplier shortage of antibiotics available to treat Strep A'.
It added: 'We sometimes have surges for products and increased demand means some pharmacies are having difficulties obtaining certain antibiotics.
'We are working urgently with manufactures and wholesalers to explore what can be done to expedite deliveries and bring forward stock they have to help ensure it gets to where it’s needed, to meet demand as quickly as possible and support access to these vital medicines.'
Meanwhile, experts have called for the UK to dish out Covid-style home testing for Strep A to detect the infection earlier, reduce the risk of severe illness and ease NHS pressures.
Dr Nicole Robb, an infectious disease expert at Oxford University, told MailOnline that community testing, at home and in pharmacies, would take the 'strain off GPs and hospitals' and let people 'rapidly test if they suspect Strep A'.
She said: 'If your child has sore throat it's likely to just be a mild infection — but in a very small number of cases it might be more serious.'
A simple saliva or nasal swab could confirm a Strep A infection 'before waiting for it to progress' or rule out the bug, easing parent worries.
Rapid and reliable testing could also see those with confirmed Strep A — or other winter bugs — stay at home and reduce transmission due to earlier detection, Dr Robb said.
'It would also mean that less antibiotics are handed out 'just in case', and we keep them for illnesses that really require them, cutting antibiotic resistance,' she said.
Dr Robb claimed such lateral flows are already being trialled in some hospitals but it 'needs to be accelerated'.
The surge in cases and resulting fears has left the NHS in 'meltdown', with parents of sick children swamping GP practices, A&E units and 111 call centres.
This is on top of normal winter pressures — which sees extra demand due to the cold weather and flu every year — and more patients needing NHS care due to spikes in flu and RSV.
The Grange University Hospital in Gwent, South East Wales, saw 90 children on Monday night, with some facing 10-hour waits, the Mirror reported.
Dr Robert Stafford, an A&E consultant at the hospital, told the newspaper: 'We know there are a lot of parents and carers who are anxious about Strep A. But I would urge people to stay calm.'
Meanwhile, the Royal Belfast Hospital for Sick Children yesterday announced that it postponed all routine procedures due to 'significant pressures' from the bacterial infection outbreak.
It said more than 200 youngster attended its emergency department on Tuesday alone.
The hospital, which treated five-year-old Stella who died from Strep A this week, said ear, nose and throat procedures are among those being pushed back.
Meanwhile, health chiefs yesterday issued guidance which suggested children with sore throats shouldn't attend school in case they have Strep A.
Department for Education bosses also list a sore throat and headaches, which can be a sign of dozens of ailments, as symptoms of the usually-harmless bug.
Its advice, put together by the UKHSA, states that those with suspected Strep A should not attend school.
Professor Livermore added: 'A child with a strep A infection certainly should be kept home and given antibiotics.
'The problem with the Government's advice is that the great majority of children with a sore throat will have a virus, not strep A. And they've missed quite enough school already.'
Most watched News videos
- Rare clip of Barron Trump talking with Slovenian accent in 2010
- Ukrainian Leopard tank takes on entire column of Russian armour
- Cruise ship passenger hit with furniture as ship tilts '45 degrees'
- Looking back at how Barron Trump began to tower over his family
- Donald Trump's historic handshake with Joe Biden at White House
- Phone snatchers terrorise London streets as notorious thefts rise
- Ukrainian drones decimate Russian tankers in Kursk counter
- Donald Trump and Elon Musk join singer Christopher Macchio onstage
- Reporters shout questions at Trump: 'How does it feel to be back?'
- Shocking moment coach father slaps Taekwondo star daughter
- CCTV captures moments before worker is 'squashed' by reversing lorry
- Spain drowns yet again as heavy streams flood streets overnight
































































































































































































































































































































































































